Discover how virtual reality is reshaping motor rehabilitation for stroke and neurological impairments by turning repetitive therapy into engaging, adaptive training. This blog explores VR-based and home-based telerehabilitation systems that use biosensors like EEG, EMG, and motion tracking to monitor recovery in real time, improve motivation, and support more accessible, personalized recovery of movement and gait.
Table of Contents
Think about reaching for an object. It feels like a simple process, yet in reality it’s a complex act. This action relies on a combination of motor acts that are processed at many different levels in the brain and body. For people with motor impairments following neurological injury, what looks to be an everyday task like eating, typing an email, reading a book, can become a challenge.
Neurological impairments may affect any part of the body. One of the most common examples is the impact on lower limb motor functions, leading to walking limitations and participation restrictions in daily life activities. The ability to perform additional motor and cognitive tasks during walking is highly affected and with it, the ability to adjust to the surrounding environment, while for instance crossing the street or stepping over an obstacle.
There are many parts of the central and peripheral nervous system involved in these processes and when one part is damaged, recovery of these motor abilities is often a cumbersome and slow process. Several strategies for recovery have been explored, including intensive rehabilitation [1], repetitive motor training [2], and mirror therapy [3], among others. Below, we will talk about the next approach.
VR-based Rehabilitation
When thinking about traditional rehabilitation, what does it come to mind? It’s boring! It is repetitive by nature, and these repetitions reduce patients’ motivation over time. Additionally, it requires (at least!) one therapist to work 1:1 with the patient, increasing the need for resources and therefore, the costs for the healthcare system. Moreover, it doesn’t provide objective data and the ability to monitor the portion of therapy patients complete at home.
Researchers are seeking novel methodologies to improve and make motor rehabilitation more engaging and effective. Virtual Reality (VR) has recently emerged as a valid addition to conventional therapy by incorporating rehabilitation strategies in a novel and low-cost approach [4]. VR-based therapy can provide a positive learning experience, and be engaging and motivating.

With VR-based therapy, tasks can be tailored to the patients’ needs, with imitation or video-game like activities. The advantage of virtual reality is that the possibilities are essentially endless. Virtual environments can be customized by designing tasks that fit the individual’s cognitive and physical impairments, which is critical in maximizing brain reorganization and reactivating those brain areas involved in motor planning, learning, and execution [5, 6], as well as in maintaining engagement.
Researchers at the University of South Carolina combine the principles of VR and Brain Computer Interface (BCI) to treat chronic stroke survivors with different levels of motor impairment [7]. Their multimodal approach uses virtual reality to show patients avatars of their upper limbs; then, combine brain (electroencephalography, or EEG) and muscle (electromyography, or EMG) sensors and signals to visualize their attempted movement to perform the presented task. Over time, this has shown to improve the patients’ motor-imagery (their ability to imagine and plan movements), re-engage the motor circuits, and improve recovery of upper limb motor functions.
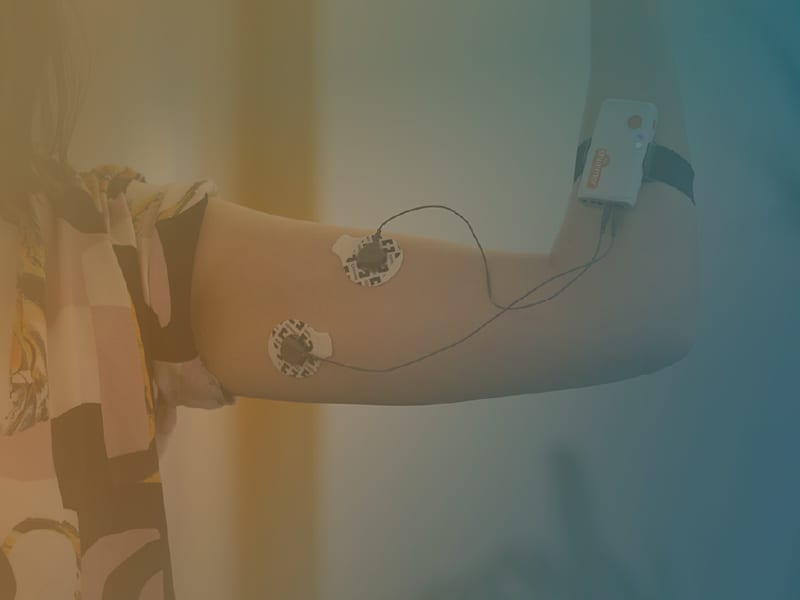
VR mediated therapy has also yielded significant improvements in gait rehabilitation following a stroke. VR interventions to retrain gait frequently comprise treadmill training systems in combination with a screen or a head-mounted device to create an immersive environment. Additional biosensors such as Inertial Measurement Units (IMUs), force sensors, and EMG sensors are also used to track progress in the patients’ kinematics, movement dynamics, and muscle activation. Real-time visualization of these parameters allows therapists to provide patients with timely feedback on the progress and quality of tasks they perform, giving them the opportunity to understand and correct possible mistakes.
Furthermore, the adjustable practice and customizable environments enable therapists to design dual tasks and unexpected situations, so that patients can relearn to adapt to environmental changes while walking. Results have shown that VR-trained patients can more effectively increase their gait speed as demanded by the task when compared to patients that underwent traditional rehabilitation. With practice, they can better adapt their gait with respect to the change in the surrounding environment [8].
To see how these concepts are applied in practice, explore our Talk to a Research Expert page.
VR-based Telerehabilitation
For stroke survivors, maintaining a daily therapy routine increases the probability of positive rehabilitation outcomes. However, millions of patients in the US and Europe live in rural areas and don’t have easy access to therapists, which can force them to choose between costly daily travel to urban areas, or foregoing the beneficial treatments.
In these conditions, maintaining the patients’ motivation becomes a challenge. Additionally, for the portion of therapy that patients complete at home, the inability to monitor their compliance with the prescribed exercise regimen makes traditional rehabilitation outcomes difficult to predict, and potentially less likely to succeed.
Today, telerehabilitation based on virtual reality is an area of active research. Therapists using VR-based telerehabilitation can prescribe exercise routines via the web which are then easily accessed and executed by patients from the comfort of their homes. VR-based tasks provide patients with a controlled environment where they can exercise. Clinical measures are collected in real time and stored in online databases, accessible remotely.
Therapists can thus monitor the patients’ progress via the web and modify the therapy as needed without real-time interaction or training. In this way, therapists are able to monitor several patients exercising simultaneously at home, a big step forward from the 1:1 paradigm of traditional methods and a big cut of costs [9, 10].
Conclusions
Virtual reality is still in its early stages of medical and rehabilitation practices and clinicians still have unresolved questions related to the technology, such as:
- Are there minimal cognitive and perceptual requirements to apply VR for sensorimotor rehabilitation effectively?
- Are semi-immersive systems as effective as immersive environments in promoting motor recovery?
However, initial results from pilot studies are highly encouraging, especially for post-stroke chronic patients, and provide insights on the effectiveness of VR-based motor rehabilitation, including:
- It provides a more advanced digital rehabilitation methods as an alternative to traditional therapy, thus maximizing the effect of rehabilitation measures.
- It allows patients with different neurological disorders to execute actions they are not able to perform in real life due to their disabilities.
- It can provide individualized treatment plans developed on the basis of careful assessment and following case-by-case treatment goals.
- It enhances patient’s engagement and motivation with 3D virtual environments and video game-like tasks.
- It provides immediate and illustrative feedback.
- It improves outcomes through neurophysiological measurements and analysis.
- It provides a controlled environment for telerehabilitation.
I hope you’ve enjoyed reading about the use of VR in rehabiliation, if you’d like to learn more about using VR devices with iMotions, download our brochure below.
Download iMotions VR Eye Tracking Brochure
iMotions is the world’s leading biosensor platform.
Learn more about how the VR Eye Tracking Module can help you with your human behavior research

References
[1] Wittenberg G.F., Richards L.G., Jones-Lush L.M., et al. (2017). Predictors and brain connectivity changes associated with arm motor function improvement from intensive practice in chronic stroke. F1000Research 2017, 5:2119. doi: 10.12688/f1000research.8603.2
[2] Thomas L.H., French B., Coupe J., et al. (2017). Repetitive Task Training for Improving Functional Ability After Stroke A Major Update of a Cochrane Review. Stroke.2017;48:e102-e103.doi: 10.1161/STROKEAHA.117.016503
[3] Pérez-Cruzado, D., Merchán-Baeza, J. A., González-Sánchez, M., & Cuesta-Vargas, A. I. (2016). Systematic review of mirror therapy compared with conventional rehabilitation in upper extremity function in stroke survivors. Australian Occupational Therapy Journal, 64(2), 91–112. doi:10.1111/1440-1630.12342
[4] Laver K.E., Lange B., George S., Deutsch J.E., Saposnik G., Crotty M. (2017) Virtual reality for stroke rehabilitation. Cochrane Database of Systematic Reviews. Issue 11. Art. No.: CD008349. doi: 10.1002/14651858.CD008349.pub4.
[5] Boyd, L. A., Winstein, C. J. (2001). Implicit motor-sequence learning in humans following unilateral stroke: the impact of practice and explicit knowledge. Neuroscience Letters, 298(1), 65–69. doi:10.1016/s0304-3940(00)01734-1
[6] Rizzo A., Kim G.J. (2005). A SWOT Analysis of the Field of Virtual Reality Rehabilitation and Therapy. Presence, Vol. 14, No. 2, April 2005, 119–146 © 2005 by the Massachusetts Institute of Technology
[7] Vourvopoulos A, Pardo OM, Lefebvre S, Neureither M, Saldana D, Jahng E and Liew S-L (2019) Effects of a Brain-Computer Interface with Virtual Reality (VR) Neurofeedback: A Pilot Study in Chronic Stroke Patients. Front. Hum. Neurosci. 13:210. doi: 10.3389/fnhum.2019.00210
[8] de Rooij I., Port I., Visser-Meily J., Meijer J. (2019). Virtual reality gait training versus non-virtual reality gait training for improving participation in subacute stroke survivors: Study protocol of the ViRTAS randomized controlled trial. Trials. 20. 10.1186/s13063-018-3165-7.
[9] Pareto L., Johansson B., Zeller S., et al. (2011). Virtual TeleRehab: A case study. Studies in health technology and informatics. 169. 676-80. 10.3233/978-1-60750-806-9-676.
[10] Tchero H., Tabue-Teguo M., Lannuzel A., Rusch E. (2018). Telerehabilitation for Stroke Survivors: Systematic Review and Meta-Analysis. J Med Internet Res 2018; 20(10):e10867. doi: 10.2196/10867. pmid: 30368437. pmcid: 6250558







